
Composite
Bonding
Composite bonding is a modern, minimally invasive way to give your teeth a cosmetic boost. It can reshape them, brighten their appearance, and rebuild areas that have been worn down — all without major dental work.
8 Week Money Back Guarantee*
Understanding Composite Bonding
Composite bonding involves the application of a highly aesthetic, tooth-coloured resin material to the enamel surface of the teeth. The resin is adhesively bonded to the tooth using modern dental bonding systems that create a micromechanical and chemical union between the material and enamel.
From a clinical perspective, bonding is:
- Additive (material is added rather than enamel removed)
- Minimally invasive
- Reversible in many cases
- Completed in a single visit in most cases
It is frequently used to:
- Improve tooth proportions
- Close small diastemas (gaps)
- Restore chipped or worn incisal edges
- Mask intrinsic staining
- Harmonise asymmetrical teeth
- Refine outcomes following orthodontic treatment such as Invisalign
- Enhance results after professional whitening
When performed with proper occlusal assessment and aesthetic planning, composite bonding can significantly improve smile balance while maintaining structural integrity.
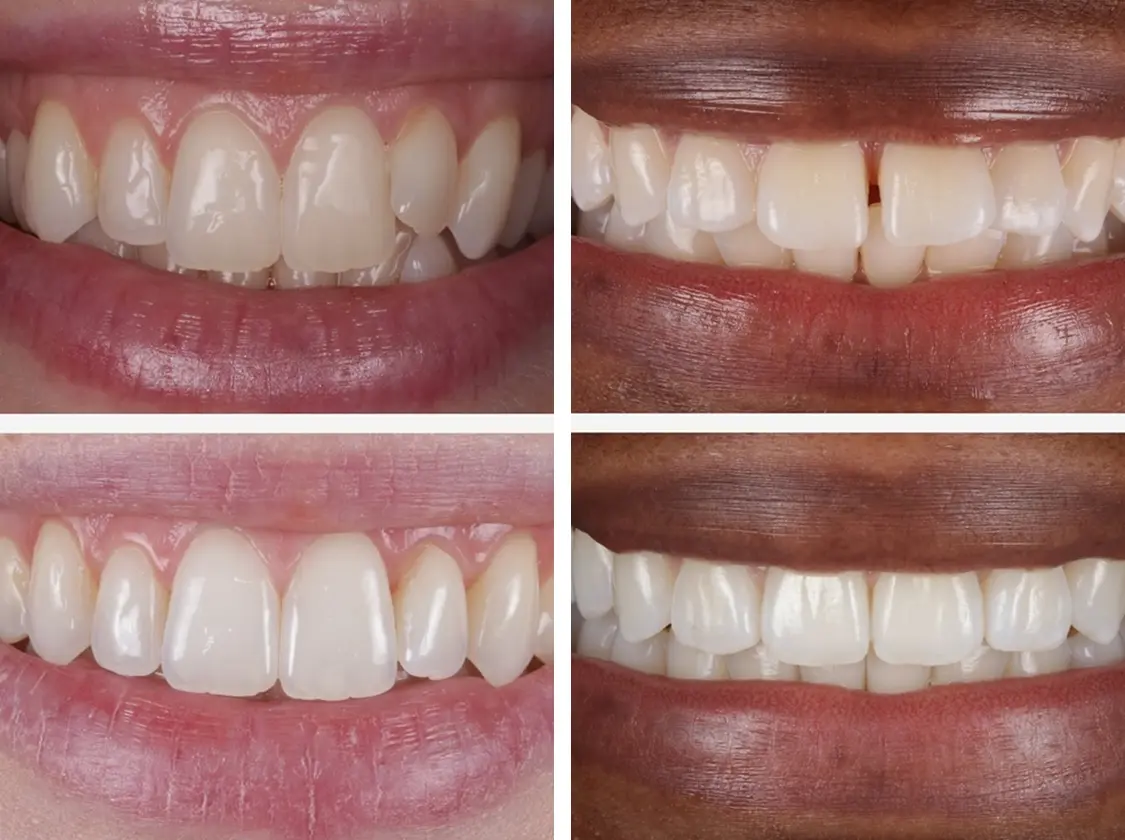
Benefits of Composite Bonding for Dental Concerns
Addressing Aesthetic Issues
From an aesthetic standpoint, composite bonding allows for precise modification of tooth morphology. The clinician sculpts the resin directly onto the tooth, adjusting:
- Length
- Width
- Line angles
- Incisal translucency
- Surface texture
- Shade gradients
Modern nano-hybrid composite materials replicate natural enamel and dentine layering, enabling highly lifelike results.
Common aesthetic concerns addressed include:
- Chipped or fractured enamel
- Uneven incisal edges
- Peg laterals
- Discoloured enamel
- Mild crowding appearance
- Small gaps between teeth
The result is improved symmetry, proportion, and facial harmony — often immediately visible at the end of the appointment.
Restoring Tooth Functionality
Beyond aesthetics, composite bonding can restore functional integrity.
Clinically, bonding may:
- Reinforce weakened enamel
- Restore minor structural loss from wear (attrition/erosion)
- Improve incisal guidance
- Re-establish proper contact points
- Protect exposed dentine
When rebuilding worn edges, careful attention is given to occlusion (bite dynamics) to prevent premature loading and ensure longevity. In cases of mild tooth wear, composite can act as a protective overlay to slow further structural loss.

The Consultation Process
What to Expect During Your Initial Visit
A comprehensive consultation is essential before treatment. This includes:
- Full clinical examination
- Photographic documentation
- Bite (occlusal) assessment
- Discussion of smile goals
- Shade analysis
- Evaluation of gum health
In some cases, digital smile design or wax mock-ups may be used to visualise the anticipated result.
Importantly, underlying issues such as active decay, gum disease, or uncontrolled bruxism must be addressed prior to bonding. Treatment planning is personalised and conservative, focusing on long-term stability rather than short-term cosmetic gain.
Tooth Preparation for Composite Bonding
The Steps Involved in Tooth Preparation
Composite bonding requires minimal preparation compared to veneers or crowns.
Typical steps include:
- Surface Cleaning – Removal of plaque and debris.
- Shade Selection – Matching composite to surrounding dentition.
- Isolation – Use of cotton rolls or rubber dam for moisture control.
- Etching – Application of phosphoric acid to create micro-retentive enamel surface.
- Bonding Agent Application – Adhesive resin placed and light-cured.
Enamel removal is usually negligible unless reshaping is required. Preservation of natural tooth structure remains a priority.
Anesthesia Options for Comfort
In most purely additive bonding procedures, local anaesthesia is not required. However, anaesthetic may be indicated if:
- Decay is present
- The bonding extends near dentine
- Significant reshaping is needed
Patient comfort is carefully assessed on a case-by-case basis.
The Composite Bonding Procedure
Applying the Composite Material
Composite resin is applied in increments to ensure proper curing and strength. The clinician:
- Builds dentine layer opacity
- Adds enamel translucency
- Mimics natural light reflection
- Controls contour and emergence profile
Each layer is cured using a high-intensity LED curing light, ensuring optimal polymerisation.
Shaping and Polishing the Bonding
Once the composite is placed, meticulous contouring follows. Fine finishing burs and polishing discs refine:
- Line angles
- Surface anatomy
- Incisal embrasures
- Gloss level
Proper polishing reduces plaque retention and enhances stain resistance. The final stage involves occlusal adjustment to ensure the bonded surfaces are not overloaded during biting or grinding.
Aftercare for Composite Bonding
Tips for Maintaining Your New Smile
Composite bonding can last many years with appropriate care.
Recommended maintenance includes:
- Twice-daily brushing with non-abrasive toothpaste
- Daily flossing
- Regular hygiene appointments
- Night guard use if bruxism is present
- Avoiding nail biting or hard object chewing
Routine professional polishing can maintain surface lustre.
Foods to Avoid After Treatment
While bonding sets immediately, it is advisable to minimise:
- Highly pigmented foods (coffee, red wine, curry) in first 48 hours
- Hard foods that may chip edges
- Sticky confectionery
- Ice chewing
Long-term, moderation rather than complete avoidance is key.
Risks and Considerations
Potential Complications and How to Mitigate Them
As with any dental procedure, composite bonding carries potential risks:
- Chipping or fracture
- Staining over time
- Marginal discolouration
- Debonding
- Wear in high-stress areas
Risk mitigation includes:
- Proper occlusal assessment
- Case selection
- Protective night guards
- Periodic maintenance
- High-quality polishing protocols
When executed correctly, complication rates are low.
Candidacy: Who Is an Ideal Candidate?
Ideal candidates typically:
- Have good oral hygiene
- Possess healthy gums
- Present with minor to moderate cosmetic concerns
- Do not have severe bite dysfunction
- Do not exhibit uncontrolled bruxism
Patients requiring major alignment correction or extensive structural rehabilitation may require orthodontics or indirect restorations instead.

Cost of Composite Bonding
Breakdown of Typical Costs
Costs vary depending on complexity and geographic region. Typically pricing is:
- Per tooth basis
- Based on number of surfaces involved
- Influenced by time and artistry required
Minor edge bonding differs significantly in cost from full smile recontouring.
Factors Influencing Overall Price
Key determinants include:
- Number of teeth treated
- Case complexity
- Need for preparatory treatment
- Clinician experience
- Materials used
- Geographic location
While composite bonding is generally more affordable than porcelain veneers, it may require maintenance over time.
Financing Options for Composite Bonding
Exploring Payment Plans
Many practices offer:
- Interest-free instalment plans
- Staged treatment options
- Third-party healthcare financing
- In-house payment scheduling
This allows patients to access aesthetic treatment without immediate full payment.
Insurance Coverage Considerations
Composite bonding performed purely for cosmetic purposes is typically not covered by insurance. However, if bonding restores function following fracture or decay, partial coverage may apply depending on policy terms.
Patients are encouraged to verify benefits directly with their provider.

Composite Bonding Testimonials
Real Experiences from Composite Bonding Recipients
Patients commonly report:
- Increased confidence
- Improved smile symmetry
- Natural-looking results
- Minimal discomfort
- Immediate transformation
Clinically, the most rewarding outcomes occur when expectations are aligned with realistic limitations and long-term maintenance is understood.
Frequently Asked Questions
With proper care, composite bonding can last 5–10 years, sometimes longer. Longevity depends on:
- Bite forces
- Oral hygiene
- Dietary habits
- Night guard compliance (if required)
Periodic refinishing or small repairs may extend lifespan.
Information
Coming Soon!